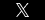Search
Insurance carriers will soon have to pay for COVID-19 at-home tests — up to 8 per person per month.
We still don’t know **clicks refresh on the Supreme Court’s website** whether the OSHA vax-or-test mandate will survive Supreme Court scrutiny.
But, in the meantime, the Biden Administration announced some big news yesterday about at-home COVID-19 tests.
Starting on Saturday, January 15, 2022, insurance companies and group health plans must cover the cost of over-the-counter, at-home COVID-19 tests, so people with private health coverage can get them for free.
According to this U.S. Department of Health & Human Services press release, “the new coverage requirement means that most consumers with private health coverage can go online or to a pharmacy or store, buy a test, and either get it paid for up front by their health plan, or get reimbursed for the cost by submitting a claim to their plan.”
Here are the details:
- Beginning January 15, 2022, individuals with private health insurance coverage or covered by a group health plan who purchase an over-the-counter COVID-19 diagnostic test authorized, cleared, or approved by the U.S. Food and Drug Administration (FDA) will be able to have those test costs covered by their plan or insurance.
- Insurance companies and health plans must cover eight free over-the-counter at-home tests per covered individual per month. That means a family of four, all on the same plan, would be able to get up to 32 of these tests covered by their health plan per month.
- There is no limit on the number of tests, including at-home tests, that are covered if ordered or administered by a health care provider following an individualized clinical assessment, including for those who may need them due to underlying medical conditions.
Under the OSHA ETS, employers can shift the costs of a COVID-19 test onto an employee. I recognize that a lot of this depends on supply, but if an employee can procure eight tests in a month, then s/he is good to go to test weekly. Plus, if these over-the-counter (OTC) tests feature digital reporting of date and time-stamped results, then employees can self-administer the test without the need to be observed by the employer or an authorized telehealth proctor. Not only does that make testing less complicated, but it cuts down on the time spent testing, which may otherwise be compensable under the OSHA ETS / Fair Labor Standards Act.
**clicks refresh on the Supreme Court’s website**
Sorry folks, yes, you need to keep planning for the OSHA ETS. But do check with your third-party administrator to ensure that your employees can procure these free tests.
 The Employer Handbook Blog
The Employer Handbook Blog